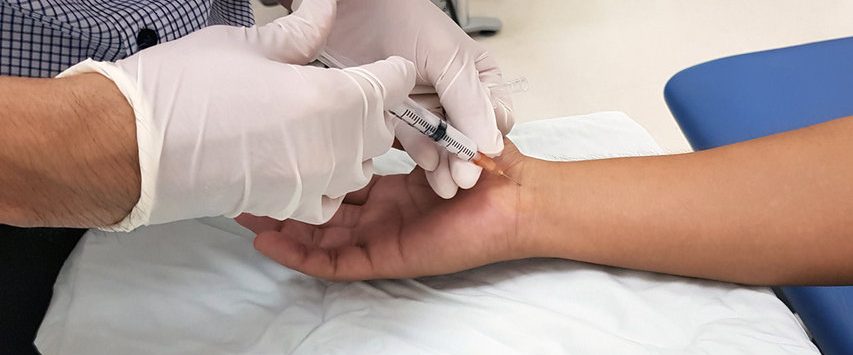
Steroid Injection Therapy
Corticosteroid injection therapy
This page explains what a corticosteroid (steroid) injection is, why it may be offered, what to expect before, during and after the procedure, common benefits and risks, alternatives, and practical advice to help you decide.
What is a steroid injection?
A corticosteroid injection delivers a strong anti-inflammatory medicine directly into a joint or into the soft tissues around a joint to reduce inflammation, swelling and pain. The injection can be given with a local anaesthetic to provide short-term pain relief while the steroid begins to act locally in the treated area.
Why it might be recommended?
Steroid injections are offered when pain and/or swelling from a musculoskeletal problem has not sufficiently improved with activity modification, physiotherapy, medication or other conservative measures. They are used for inflammatory conditions (for example some forms of arthritis), painful tendon or bursal condition to reduce pain and swelling.
Expected benefits and how long they last
Most people notice reduced pain and improved function within 48–72 hours but this can take up to three weeks. The duration of benefit is variable: for some people a few weeks, for others several months. Some patients gain little or no benefit; results cannot be guaranteed and depend on the underlying condition and degree of inflammation.
How the procedure is performed
- I will explain the procedure and check your medical history before taking consent.
- The skin is cleaned and the area may be numbed with a local anaesthetic or cold spray. The steroid (which can be combined with local anaesthetic) is injected into the target joint or soft tissue.
- The procedure is usually quick and can be done during your initial or follow up appointment. It is normal to be advised to relative rest for a couple of days after the injection to allow the medication to work.
Common and important risks
- Short-term increase in pain or “flare” for 24–72 hours after the injection is common and usually settles with rest and simple pain relief.
- Temporary rise in blood sugar may occur for a few days for people with diabetes; closer glucose monitoring may be recommended.
- Infection at the injection site or deeper in the joint is very rare but can be serious and requires urgent attention.
- Tendon weakening or, rarely, tendon rupture can happen, particularly if the injection is close to a tendon that is already damaged.
- Local skin changes such as thinning, dimpling or loss of skin colour at the injection site can occur and may be permanent.
- Facial flushing, mood changes or temporary systemic effects are possible but usually short lived.
- Steroid injections may delay elective joint surgery for up to several months in some circumstances; discuss timing with your clinician if surgery is planned.
Each of these risks will be reviewed with you before you give consent.
Who should not have an injection (important precautions)
- Signs of infection at or near the injection site, or a significant systemic infection.
- Known allergy to a steroid or the local anaesthetic planned for use.
- Certain recent or planned surgical or dental procedures; your clinician will advise about timing because injections can affect surgical planning in some cases.
- Pregnancy or other medical conditions may alter suitability; tell your clinician about pregnancy, breastfeeding, diabetes, immune-suppressing medication, or blood-thinning medicines before the injection.
Before and after the injection — practical advice
- You will be advised whether to stop or alter your medication following discussion with me; bring a list of current medications and any allergies to your appointment.
- Plan to rest the treated area for 24–48 hours after the injection and avoid strenuous activity for a short period; follow any specific exercise or physiotherapy advice you are given.
- If you develop increasing pain, fever, spreading redness, new weakness, or other worrying symptoms after the injection, contact the clinic or seek urgent medical attention because these can be signs of complications such as infection or tendon rupture.
Alternatives
- Continued physiotherapy and exercise programmes, analgesic and anti-inflammatory medications, orthoses or activity modification.
- For some conditions, other interventions (e.g., injection of other agents, referral to specialist services, or surgical options) may be appropriate. I will discuss alternatives relevant to your diagnosis and goals.
Frequently asked questions
- Will the steroid affect the rest of my body?
The steroid acts mainly where it is injected; only a small amount reaches the rest of the body, so systemic effects are usually limited and short lived. - How many injections can I have?
This depends on the joint or tissue, clinical need, and your response. Clinicians typically limit frequency to avoid cumulative effects and will discuss a plan with you.
Consent and shared decision-making
I will explain the expected benefits, likely duration of effect, and the risks specific to your condition and the site to be injected. You will have the opportunity to ask questions and to either accept or decline the procedure. If you decide to proceed, we will ask you to give informed consent before the injection.
Contact and who to speak to
If you have questions before your appointment, practical concerns about preparation, or symptoms after the injection you are worried about (fever, increasing pain, redness, swelling, new weakness), contact me promptly. If you develop severe symptoms outside clinic hours, seek urgent or emergency care.
